In 2024, nearly 64% of all Legionnaires' disease cases in England and Wales involved individuals aged 60 and over, placing your residents at the very center of the risk profile. Managing these risks isn't just about routine maintenance; it's about fulfilling your legal duty under the Health and Safety at Work Act 1974 and meeting strict CQC expectations. Understanding the specific care home legionella policy requirements for 2026 is the only way to protect your vulnerable residents and safeguard your facility from the "Inadequate" ratings or heavy fines that follow a compliance failure.
You likely feel the pressure of balancing ACOP L8 technicalities with the healthcare-specific demands of HTM 04-01. It's a complex landscape where a single missed temperature check can lead to significant penalties, much like the £1.5 million fine Bupa Care Homes faced following a 2025 appeal. We're here to transform that regulatory burden into a sense of security. This guide provides a definitive roadmap to bridge the gap between technical HSE standards and clinical care requirements. You'll learn the exact 2026 temperature thresholds, record-keeping mandates, and the documentation needed to ensure total peace of mind during your next inspection.
Key Takeaways
- Align your water safety protocols with the dual expectations of the CQC and HSE to secure your facility's regulatory standing and avoid heavy penalties.
- Establish a clear management hierarchy and documentation framework to meet all care home legionella policy requirements for the 2026 inspection cycle.
- Master the balance between scalding prevention and bacterial control by implementing specific maintenance schedules for TMVs and assisted bathing assets.
- Maintain a continuous state of readiness through a structured written scheme that prioritizes monthly temperature monitoring and quarterly disinfection.
- Utilize independent compliance audits to satisfy the "Well-Led" criteria and gain professional, third-party verification of your water safety systems.
The Legal Framework: Why Care Homes Face Stricter Legionella Requirements
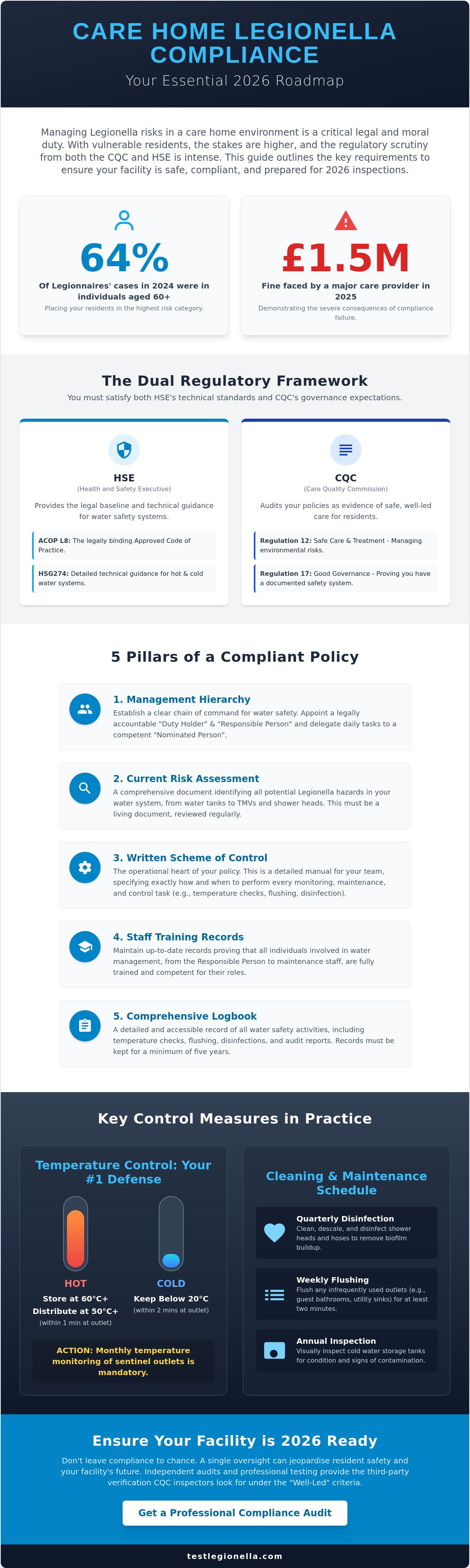
Care homes operate under a regulatory microscope that most businesses never experience. You aren't just managing a building; you're protecting a population that is uniquely susceptible to waterborne pathogens. According to 2024 UKHSA data, individuals aged 60 and over accounted for nearly 64% of all legionellosis cases in England and Wales. This high incidence rate is why the dual-regulatory environment of the Health and Safety Executive (HSE) and the Care Quality Commission (CQC) is so demanding. Meeting care home legionella policy requirements isn't a suggestion; it's a fundamental pillar of your license to operate.
While the HSE's ACOP L8 provides the legal baseline for all UK businesses, care facilities must often look toward HTM 04-01. This healthcare-specific guidance addresses the needs of immunocompromised residents, where even low levels of bacteria can be fatal. Failing to bridge the gap between these standards invites catastrophic consequences. In 2025, a major care provider's fine was finalized at £1.5 million following a Legionella-related death. Beyond the financial impact, a single failure can trigger CQC "Special Measures," effectively putting your facility's future at risk. For a deeper look at the medical risks your policy must mitigate, you can review this Legionnaires' disease overview.
CQC Regulation 12 and Regulation 17
Regulation 12 focuses on "Safe Care and Treatment," requiring you to manage environmental risks to prevent harm. However, many managers fail to prioritize Regulation 17, which mandates "Good Governance." This requires a formal, written record of your management systems. During an unannounced inspection, your written policy serves as the primary evidence of compliance. It proves you don't just react to problems; you have a proactive, documented strategy for resident safety that ensures accountability at every level of your organization.
HSE ACOP L8 and HSG274 Compliance
The HSE's Approved Code of Practice (ACOP L8) has a unique legal status. If you're prosecuted for a safety breach, you'll need to prove you followed this code or an equally effective alternative. Under this framework, you must appoint a "Duty Holder" and a "Responsible Person" with the competence to oversee water safety. Technical guidance in HSG274 Part 2 outlines the specific controls for hot and cold water systems. Integrating these technical standards into your care home legionella policy requirements ensures that your maintenance staff has a clear, legally-defensible roadmap for daily operations.
Mandatory Components of a Care Home Legionella Policy
A robust policy transforms regulatory pressure into operational clarity. It ensures every staff member knows their specific role in preventing outbreaks. To meet the full spectrum of care home legionella policy requirements, your document must include five core pillars: a management hierarchy, a current risk assessment, a written scheme of control, staff training records, and a comprehensive five-year logbook. These elements work together to provide the "Good Governance" evidence that CQC inspectors prioritize under Regulation 17.
The written scheme of control is the heart of this framework. It acts as a detailed manual for your maintenance team, specifying exactly how and when to perform every safety task. Without this level of detail, your policy is just a statement of intent rather than a functioning safety system. Maintaining these records for at least five years is a non-negotiable legal requirement that proves a history of consistent care. If your current documentation feels fragmented, securing professional Legionella compliance testing can help you establish a clean, compliant baseline for 2026.
Defining Roles and Responsibilities
The Registered Manager typically serves as the "Responsible Person," holding legal accountability for the water system's safety. They must delegate daily operational tasks to a "Nominated Person" who acts as the primary on-site lead for water checks. When you hire external contractors for technical tasks, ensure they are UKAS accredited to guarantee the validity of your data. Clear accountability prevents the "compliance gap" where critical tasks are missed because staff members assume someone else is responsible.
The Risk Assessment as a Living Document
A static PDF gathering dust on a shelf won't satisfy a modern inspection. You must treat your risk assessment as a living document that evolves with your facility. While a review is required at least every two years, you need an immediate update if you modify the plumbing, change building usage, or suspect your current controls are no longer effective. Integrating foundational what is legionella knowledge into your staff induction process demonstrates a proactive safety culture. This educational approach aligns with international Legionella control regulations and guidelines, ensuring your team understands the high-stakes risks involved in their daily routines.
- Management Hierarchy: Clearly defined roles from Duty Holder to Nominated Person.
- Competence Evidence: Training certificates for all staff performing water checks.
- Remedial Action Plans: Documented proof of how you've fixed identified risks.
- Asset Register: A complete list of all water outlets, tanks, and TMVs.
Managing High-Risk Assets: TMVs and Assisted Bathing
You face a constant balancing act between thermal safety and bacterial control. To prevent scalding, water at the point of use must not exceed 44°C for vulnerable residents. However, Legionella thrives in temperatures between 20°C and 45°C. This creates a paradox where the very devices used to protect residents from burns can become breeding grounds for bacteria. Your care home legionella policy requirements must explicitly address how you manage this conflict without compromising safety on either front. It's about finding the sweet spot where residents stay safe from both heat and infection.
Managing high-risk assets requires a structured approach that moves beyond simple temperature checks. You need to account for specialized clinical sinks, assisted baths, and complex blending valves that are common in modern care environments. These assets often have intricate internal pipework that can easily harbor biofilm if not maintained with precision. By integrating specific asset management protocols into your policy, you transform a complex technical challenge into a repeatable, stress-free routine for your maintenance team.
Thermostatic Mixing Valve (TMV) Maintenance
TMVs are essential for safety, yet they're high-risk areas for bacterial colonisation. Because they blend hot and cold water, they often hold stagnant, lukewarm water that is ideal for Legionella growth. Your policy must mandate annual fail-safe testing to ensure the valve shuts off immediately if the cold supply fails. Beyond testing, internal components require regular cleaning and descaling. You should document every TMV location on a site schematic drawing to ensure no hidden asset is overlooked during your annual maintenance cycles.
Assisted Baths and Sensory Rooms
Specialized equipment like assisted baths and sensory room features often present "dead legs" in your plumbing system. These occur when pipework is infrequently used, allowing water to stagnate and reach dangerous temperatures. If an en-suite room is empty during resident turnover, you must implement a strict flushing regime to keep water moving. Spa or whirlpool baths carry an even higher risk because the mechanical action of the jets significantly increases the risk of aerosolisation, which is the primary route for Legionnaires' disease transmission. Your policy should clearly outline the disinfection protocols for these high-aerosol assets.
In some scenarios, you might need to implement Point-of-Use (POU) filtration. These specialized filters attach directly to taps or showerheads to provide an immediate barrier against bacteria. They're typically necessary for residents who are severely immunocompromised or as a temporary safety measure following a positive test result. While POU filters offer rapid protection, they should be viewed as a secondary defense rather than a replacement for robust, system-wide temperature control and regular maintenance.
Implementing the Written Scheme: Monitoring and Maintenance
Operational excellence is where your safety strategy meets reality. Your written scheme shouldn't be a dormant file; it's a live schedule that dictates the daily rhythm of your maintenance staff. Meeting care home legionella policy requirements hinges on the consistency of these checks. By following a structured monitoring program, you eliminate the guesswork and create a robust audit trail that satisfies both HSE inspectors and CQC assessors. This proactive approach transforms a complex legal burden into a manageable, professional routine.
Temperature control remains your primary defense against bacterial growth. You must ensure that hot water is stored at a minimum of 60°C and distributed so that it reaches at least 50°C (or 55°C in healthcare-specific areas) within one minute at the outlets. Conversely, cold water must remain below 20°C. If these thermal boundaries slip, Legionella can rapidly colonise your system. Regular monitoring allows you to identify these shifts early, protecting your residents and your reputation before a minor fluctuation becomes a major risk.
Standard Monitoring Frequencies
Consistency is the backbone of compliance. Your policy must mandate specific intervals for every check to ensure nothing is overlooked. Follow these standard frequencies to maintain a compliant water system:
- Monthly: Check flow and return temperatures on calorifiers to verify 60°C storage.
- Monthly: Test sentinel point temperatures. These are the hot and cold outlets furthest and nearest to your water source.
- Quarterly: Descale and disinfect all showerheads and hoses to remove the scale and biofilm that harbor bacteria.
- Annually: Inspect cold water storage tanks for debris, stagnation, or signs of thermal gain.
Sampling and Remedial Actions
Monitoring tells you the system is under control, but legionella testing provides the scientific proof. You should move to laboratory analysis if your temperatures consistently fail, if you're managing a high-risk outbreak, or if you've recently modified your plumbing. Lab reports will show "cfu/l" (colony forming units per litre). If results exceed 100 cfu/l, you must review your risk assessment immediately. If they exceed 1,000 cfu/l, your policy must trigger a 48-hour response rule. This ensures you isolate the source, perform a chemical or thermal disinfection, and protect your residents without delay.
Don't leave your facility's safety to chance. Secure your compliance today by booking our professional Legionella compliance testing and ensure your records are inspection-ready.
Compliance Audits and Professional Testing Services
Independent validation is the final step in securing your facility's safety. While internal logs form the foundation of your defense, they shouldn't be the only layer. Meeting the full scope of care home legionella policy requirements requires a level of technical scrutiny that most internal maintenance teams simply don't have the tools to provide. An external audit acts as a professional seal of approval, transforming your internal processes into a robust, legally defensible framework that satisfies the most demanding CQC inspectors.
CQC inspections under the "Well-Led" criteria focus heavily on governance and accountability. They want to see that you've sought specialist expertise to verify your systems. This is where "DIY" policies often crumble; they frequently lack the technical anchors and site-specific nuances required to survive a legal inquiry. When you factor in the potential for unlimited fines or a "Special Measures" rating, understanding the legionella risk assessment cost in 2026 becomes a strategic investment in your facility's longevity and reputation.
The Value of an Annual Compliance Review
An annual review allows you to move beyond the absolute acop l8 minimums. It's about resident safety and operational peace of mind. Professional reports simplify the CQC evidence-gathering process by providing a clear, concise summary of your compliance status. These audits are designed to identify "blind spots" in your internal logs, such as missed TMV cleanings or thermal gain in cold water tanks that your team might've overlooked during busy shifts. It's a proactive way to ensure your policy remains a living, breathing document rather than a static file gathering dust.
Partnering with a Specialist
Choosing the right partner is critical for care groups with multiple locations. You need a provider that offers UK-wide national coverage to ensure consistency across your entire portfolio. At Test Legionella, we understand the sensitive nature of your environment. Every one of our testers carries appropriate DBS clearance, ensuring they can work safely and professionally around your residents. We provide the expertise you need to navigate the maze of safety regulations without the stress. Don't wait for an inspection to find a flaw in your system. Secure your care home today with a professional Legionella assessment and let us transform your regulatory burden into a sense of total security.
Secure Your Facility’s Future with Expert Water Safety
Transitioning from regulatory confusion to total operational security is a choice you can make today. By integrating the mandatory management hierarchies and technical monitoring schedules we've discussed, you move beyond mere compliance toward a culture of genuine safety. Meeting care home legionella policy requirements doesn't have to be a source of stress; it's a structured process that protects your most vulnerable residents while safeguarding your professional reputation. Consistency in your written scheme and annual audits ensures that your facility remains a safe haven.
Our specialist team is ready to help you navigate these high-stakes requirements with ease. We provide UKAS accredited laboratory analysis and professional assessors who are fully DBS-checked for your peace of mind. You'll receive CQC-ready compliance reports that turn complex technical data into clear, actionable evidence for your next inspection. This professional validation removes the guesswork and provides a definitive roadmap for your maintenance staff.
Take the first step toward a simpler, safer management routine. Book Your Care Home Legionella Compliance Audit today and let us transform your regulatory burden into a sense of total security. You've built a facility dedicated to care; let us help you protect it with expert precision.
Frequently Asked Questions
How often should a care home Legionella risk assessment be reviewed?
You must review your Legionella risk assessment at least every two years to remain compliant with HSE guidance. However, you need an immediate review if you make changes to your water system, modify building use, or suspect your current controls are no longer valid. This proactive approach ensures your safety protocols remain current and effective for your resident population, especially those who are elderly or immunocompromised.
Is it a legal requirement to have a written Legionella policy in a care home?
Yes, a formal written policy is a mandatory legal requirement for demonstrating compliance with CQC Regulation 17. Your documentation serves as the primary evidence of "Good Governance" during unannounced inspections. A robust care home legionella policy requirements framework protects you from fixed penalty notices, which can reach £4,000 for providers as of February 2025. This policy effectively transforms technical HSE standards into a clear, manageable plan.
What water temperatures should care homes maintain for Legionella control?
Maintain hot water storage at a minimum of 60°C and ensure distribution temperatures reach at least 50°C within one minute at all outlets. In healthcare-specific settings, this requirement often increases to 55°C to protect highly vulnerable residents. Cold water must stay below 20°C throughout the entire system. These thermal boundaries are your most effective defense against bacterial colonisation and are a primary focus during safety audits.
Does the CQC check Legionella records during inspections?
The CQC scrutinizes water safety records to assess if a facility meets the "Safe" and "Well-Led" criteria. Inspectors specifically look for a clear, five-year audit trail of temperature logs, risk assessments, and documented remedial actions. Failing to produce these records during an unannounced inspection can result in a "Requires Improvement" or "Inadequate" rating, which is often accompanied by significant financial penalties and increased regulatory oversight.
Who is the "Responsible Person" for Legionella in a nursing home?
The Registered Manager is typically appointed as the "Responsible Person" for water safety in a nursing home setting. They hold the legal duty to ensure all control measures are implemented, monitored, and documented correctly. While they can delegate daily tasks to a "Nominated Person" or an external contractor, the ultimate accountability for resident safety and regulatory adherence remains with the manager. This role requires a thorough understanding of current health and safety law.
How often do TMVs need to be serviced in a care facility?
Service your Thermostatic Mixing Valves (TMVs) at least once every twelve months to ensure they're functioning correctly. This annual maintenance must include fail-safe testing to prevent scalding and internal cleaning to remove bacterial biofilm. Documenting these services and their specific locations on a site schematic is a critical part of your care home legionella policy requirements and your overall water safety strategy.
What happens if Legionella is found in a care home water system?
If you detect Legionella, you must follow the emergency procedures outlined in your written scheme of control immediately. This involves isolating high-risk outlets, performing a thermal or chemical disinfection, and conducting follow-up sampling to verify the system is clear. You're required to respond to high counts (over 1,000 cfu/l) within 48 hours to ensure resident safety and maintain compliance with your legal obligations.
Can care home maintenance staff do their own water testing?
Internal maintenance staff can perform routine temperature monitoring and monthly flushing, but laboratory analysis must be conducted by a UKAS-accredited facility. Professional testing provides the scientific validation required to prove your system is safe during a legal inquiry. Relying on external specialists for sampling ensures your data is accurate, independent, and legally defensible, giving you total peace of mind during CQC inspections.




